
As a Health and Wellness Coach who happens to have a 40 year background as a Dental Hygienist behind me, it is not surprising that my interest in the link between oral and systemic health and disease has been piqued.
Gum disease, used to be seen as a localised issue, a condition that only affected the tissues within the mouth, but the truth is much more complex. There is an ever increasing amount of research that demonstrates that gum disease is deeply connected to whole body health. What happens in the mouth, does not stay in the mouth - It has far reaching consequences on the entire body.
As a Health and Wellness Coach, I take a holistic approach to wellbeing, and recognise that stress, inflammation and imbalances anywhere within the body impact upon physical, mental, and emotional health. Gum disease is indeed a powerful example of how a seemingly minor health issue can ripple throughout the entire body, affecting not only whole body health, but resilience and vitality too.
In this blog, I am going to explore the holistic link between oral disease and systemic health, and how stress plays a role. I am also going to look at what you can do to protect both your oral and overall wellbeing.

GUM DISEASE IS MORE THAN JUST BLEEDING GUMS
Gum disease is an inflammatory condition that that affects the tissues surrounding the teeth. There are two main stages:
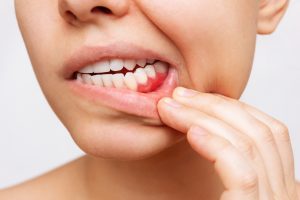
- GINGIVITIS - The early, reversible stage with red, swollen gums that bleed easily.
- PERIODONTITIS - A more advanced, irreversible stage where bacteria destroys the fibres, ligaments and bone support, leading to potential tooth loss. This stage can be managed and stabilised with the right treatment and care.
THE LINK BETWEEN HEALTH AND THE ORAL MICROBIOME
The mouth contains a community of bacteria called the oral microbiome. When balanced, it helps to protect your teeth and gums. However, poor hygiene, stress, hormonal imbalance and poor nutrition can create imbalance, leading to inflammation that affects not just the mouth, but the whole body.
PERIODONTITIS, INFLAMMATION AND THE SYSTEMIC LINK
Emerging evidence demonstrates the relationship between periodontitis and systemic disease through one common factor - Inflammation, and as an inflammatory condition, periodontal disease has been linked to over 55 different inflammatory conditions, including:
- Cardiovascular disease - bacteria from the mouth enters the bloodstream, triggering inflammation that can lead to clogged arteries.
- Alzheimer's disease - Specific disease causing bacteria and their toxic byproducts can travel to the brain, possibly contributing to cognitive decline and Alzheimer's disease.
- Respiratory diseases - Disease causing Bacteria can be inhaled in tiny droplets of saliva or travel in the bloodstream to the lungs increasing the risk of inflammatory lung diseases such as pneumonia, asthma, and COPD.
- Rheumatoid arthritis - Disease causing bacteria in periodontitis trigger an auto-immune response that targets inflammation within joints. Patients with RA also have a higher incidence of periodontal disease.
- Type 2 Diabetes - Gum disease makes diabetes harder to control, and diabetes increases gum disease risk.
- Inflammatory bowel disease - harmful bacteria from the oral microbiome can be swallowed in the saliva causing imbalance within the gut microbiome. It can also pass into the gut through the bloodstream and immune cell migration.
- Cancers - including oral cancer, lung cancer, stomach, oesophageal, breast and gall bladder cancers.
- Adverse pregnancy outcomes - pregnant women with periodontitis may have a higher risk of pre-term birth and low weight births.
- Aging - weakens the immune system and together with increased inflammation makes it easier for bacteria to cause disease. An increased risk of Osteoporosis as women get older can manifest in loss of jaw bone predisposing to an increased risk of tooth loss, and physically, loss of manual dexterity can make harder for elderly patients to clean their teeth.
- Obesity - leads to low grade systemic inflammation and altered immune responses triggered by an increase of inflammatory byproducts from fat cells, leading to increase gum inflammation and tissue destruction and bone

HOW STRESS WORSENS ORAL HEALTH
When stressed, people neglect self-care, skip brushing, and make unhealthy choices like smoking, excess alcohol and eating sugary and processed foods. Stress also weakens the immune system and triggers low grade inflammation making gum disease worse. Grinding teeth, jaw pain and mouth ulcers are other stress-related issues.
A HOLISTIC APPROACH TO MANAGING GUM DISEASE
Treatment for oral health disease should ideally follow a clinical and holistic pathway, and must always start with diagnosis and treatment of the disease by dental professionals. Beyond this, there are a range of lifestyle changes that can be addressed that can complement clinical treatment:
- Supporting Home - Care - with improved oral hygiene practices that will help you to manage your disease at home - the most important aspect of disease management.
- Smoking Cessation - stopping smoking is a huge step forward in supporting oral and whole body health as well as reducing the risk of oral and lung cancers.
- Nutritional Guidance - Anti-inflammatory foods help to manage and reduce systemic inflammation and support the immune system.
- Stress Management - Reducing stress lowers inflammation and boosts vitality and resilience.
- Sleep Management - Helps your body to heal and fight infections.
- Habit Change - support in transforming habit and behaviour change can be an enormous support on improving health and whole body wellbeing
- Building Confidence - Oral health affects how you feel about yourself and how you show up in the world. Managing gum disease can have a huge impact on supporting your self-esteem and confidence.
Your oral health is not just about your mouth. It reflects your overall health and wellbeing. By prioritising your mouth's health, you are supporting your entire body, boosting your resilience and improving the quality of your life.

